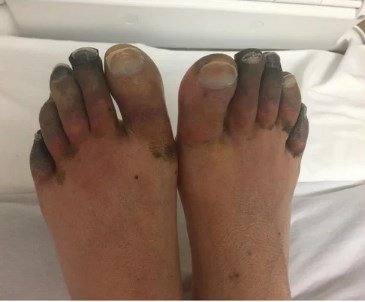
Gangrene
Gangrene means the death of the cells that is caused by infection or lack of blood circulation to the cells. It mainly occurs in the lower extremities and skin due to reduced blood flow. Your well-being is our priority. Begin your journey to health and vitality with Dr. Ruchi at 247Homeopathy Clinic.
It also occurs in the feet, fingers, toes, and muscles or in the internal organ of the body.
Types:
1. Dry gangrene: it is also known as mummification. It is most commonly associated with diabetes mellitus. It is a Slowly progressive disease and doesn’t have the involvement of the bacterias. Because it is not infectious it is not as emergent as gas gangrene or wet gangrene because there is no risk of sepsis. It occurs due to peripheral arterial disease. The affected part is dry, scaly, and shrunken and there is a demarcation line in the viable tissue or nonviable tissues where gangrenous tissues fall out automatically called autoamputation.
2. Wet gangrene: it is also known as moist gangrene or bacterial gangrene. In this, tissues are affected by bacterias that play a very important role in the decaying of tissues. It can be fatal because of the risk of sepsis as there is direct contact of the infected fluid with the circulatory fluid. It appears as blisters and gets ruptured.
Rupturing of the skin leads to ulceration. There is pus formation in the affected part with a foul smell. It occurs due to blockage of blood flow and stagnant blood is the favorable environment for the
bacterias to grow. The affected tissue becomes putrid and rotten with an offensive smell.
3. Gas gangrene: It is the bacterial infection of the tissues mainly caused by clostridium bacteria. The clostridium bacteria release the toxins that cause cell death and release gas. Gas gangrene has a high fatality rate as compared to wet gangrene. Gas gangrene can cause sepsis and shock conditions.
Causes : It is caused by the reduced blood supply to an area of the body. This can occur due to :
• Vascular problems like diabetes and peripheral arterial disease.
• Hypotension
• Severe burn and scalds
• Frostbite
• Raynaud’s disease
• Injury of the cells
• Embolism
• Smoking
• Obesity
• Excessive alcohol intake can damage the nerves
• Intravenous drug use.
Symptoms:
• Blackish bluish discoloration of the affected part of the skin.
• Inflammation of the affected part.
• Putrefaction with an offensive smell of the affected part in wet or gas gangrene.
• Dry scaly skin in dry with the demarcation line
• between viable or nonviable tissues is the characteristic sign of dry gangrene.
• Diabetic neuropathy
• Fever and chills
• Blisters with brown-red fluid in it
• Crepitus on examination due to movement of gas in the gas gangrene.
Diagnosis:
• Blood test to rule out an infection
• Fluid and tissue cultures of an infected area to see which microorganism has caused the infection.
• Blood culture to rule the growth of bacterias
• MRI or CT scan to see the blockage of blood vessels.
Homeopathy management:
• Secale cor: Secale cor is well indicated for dry gangrene.
The affected area is bluish in color and there is numbness of the affected part. It feels icy cold when touched.
Covering the affected area is intolerable.
• Anthracinum: it is best indicated for wet gangrene. Bluish and blackish discoloration of the affected part with offensive discharge. Burning sensation of the affected area. The patient feels weak. Anthracinum can be given in burns and scalds.
• Lachesis: it is also indicated for wet gangrene where purplish or blackish blisters appear over the affected part of the skin and leads to the destruction of the cells. The affected area is very sensitive to touch. There is a burning sensation in the affected part of the body.
• Carbo veg: it is well indicated in aged people with insufficient blood supply due to blocked arteries.
There is a putrid odor from the gangrenous area.